Our Telemedicine ‘robots’ used at Liverpool Women’s and Alder Hey children’s hospitals featured in The Guardian – read the piece here.
We have also reproduced the article below:
Hospital robots will save the lives of hundreds of premature babies
The technology is already enabling consultants to work at multiple sites at once, saving vital time.
Hundreds of premature babies could be saved by using new technology trialled during the pandemic that will allow doctors to treat them remotely, leading doctors say.
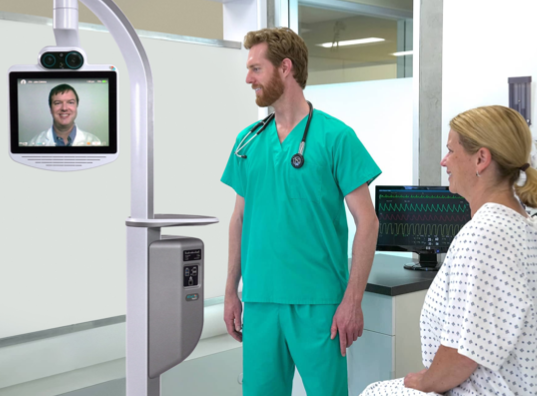
Telemedicine “robots” that enable consultants to make bedside video calls have been used at Liverpool Women’s and Alder Hey children’s hospitals to treat sick babies.
Now the head of the hospitals’ neonatal unit is putting together plans to use the Teladoc devices, so that specialists can use their expertise to help teams at smaller hospitals treat children, even in emergencies.
Dr Chris Dewhurst, the clinical director of the Liverpool Neonatal Partnership, said: “This definitely has the potential to save the lives of extremely preterm infants who were born outside of specialist centres, and improve their outcomes.
“What we’ve demonstrated is that it’s easy to use, it improves the quality of care for babies and their families, improves the speed of review, and it is very close to being there in person.”
The device, which sits on a mobile frame, has cameras, a screen and even a stethoscope, and can also link to MRI scanners and thermal-imaging cameras. It allows a consultant watching from elsewhere to view a patients’ medical records on the spot.
Dewhurst and his team began using two of the devices in March 2020. “We lost seven of our 14 consultants due to shielding or isolation – 40% of the time available for clinicians to be in hospital. It [the robot] kept us going.”
On some occasions, using the robots was better than being there in person, because the device has a camera on a boom that can be placed above the baby to show what’s happening, he said. “If I was there in person, I wouldn’t be able to see that because there were people around the baby.”
About 90,000 babies a year in England need some sort of specialist care after they are born. There are 54 Neonatal Intensive Care Units (NICUs) such as the one in Liverpool that treat the most serious cases of premature babies and those with serious conditions. Another 83 hospitals have Local Neonatal Units (LNUs) that offer short-term intensive care. And there are 44 Special Care Baby Units for monitoring the least serious cases.
Doctors try to identify which foetuses might require help after birth, but that is not always possible, and 9,523 babies needed to be transferred between hospitals at least once in 2015, according to figures from the National Neonatal Audit Programme compiled by Bliss, the charity for babies born sick or prematurely.
“For babies who are extremely preterm, and have not been able to move into an NICU, then they’re not going to be looked after by people with the specialist skills. And we know that those babies have worse outcomes,” Dewhurst said.
He is bidding for funding for the devices in hospitals with SCBUs so that clinical teams can call on specialist advice quickly.
“We now need to find the funding so that babies who were born in other hospitals who need immediate intervention can have an neonatologist there immediately, within minutes, rather than them not being there at all, because they’re 40 to 50 miles away.”
A similar system has been run by the Mayo clinic in Rochester, Minnesota, where neonatologists support teams at 19 regional hospitals.
Dr Jennifer Fang, medical director for the Mayo Clinic’s teleneonatology programme, said that only babies in a critical condition needed to be transferred, and fewer parents had to go through the stress of being separated from their babies.
“What we’ve observed is that the odds of a baby needing a transfer to a higher level of care or transfer to a hospital with an NICU are reduced by anywhere from 30 to 50%,” she said.
With difficult births or injuries to babies during birth, the Mayo specialists have a target to be on hand for remote consultations within five minutes.
Before the programme, the clinic was involved in birth-injury lawsuits about every eight to nine months, Fang said. “Now that our programme’s in place, we haven’t had a single birth-injury case for the last eight years.”
A study by the clinic showed that having neonatologists involved remotely meant that clinical teams in smaller hospitals were less likely to be overwhelmed by the complexity of dealing with a sick baby. Babies were more likely to have checks on temperature, breathing and glucose levels.
Jonathan Patrick of Consultant Connect, which supplied the robots, said the devices could be used in other circumstances. “It allows you to have access to clinicians, for example, who have retired but still want to be part of the workforce, yet can’t go to hospital every day.”
A trial is underway at University Hospitals Leicester NHS Trust where consultants doing elective surgery are often split across two sites. Dr Steve Jackson, who is running the trial, said that consultants on different sites could dial in to a consultation and discuss the case on the spot rather than doing separate ward rounds.
