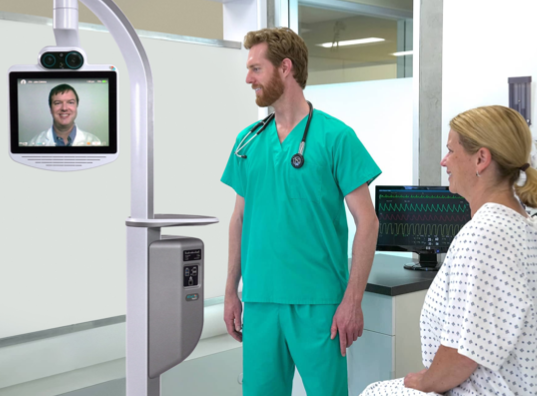
‘With the telemedicine device, I can be doing a ward round on one site in the morning and have a clinic booked immediately afterwards in the afternoon at another.’
Elective care consultants in the NHS often have to divide their time between different locations, which leads to wasted time on travel.
With telemedicine devices, consultants can see, hear, and talk to patients as if they were right beside them, even from a different hospital.
Dr Steve Jackson, a Consultant Physician and Chief Medical Information Officer at University Hospitals Leicester, frequently travels between two sites, so he was eager to test the technology.
Getting started with the new technology
The device was used for the first time when a colleague was self-isolating, and Dr Jackson could not get to the other hospital in time to cover his colleague’s ward round. Using the telemedicine device, he conducted the ward round from the hospital where he was based, and this gave him an extra 45 minutes of patient-facing time. He led the ward round from his office and commented:
‘Everyone loved it. It amazed me how easy it was to use. I had one screen with the patient visible, and then I had all the electronic patient records and the GP record open on my other screen, so I could answer questions patients asked without having to leave the bay and go back to the computer or back to the notes, so I could do it all efficiently with the junior doctors examining the patients as necessary.’
If a self-isolating clinician is well enough to work, they can still participate in ward rounds and patient consultations from home via a secure login to the telemedicine device.
Device functionality
The telemedicine device has two high-definition cameras for scans, temperature readings, and reading bedside notes. Powerful batteries allow it to run off-power for four hours. It is height-adjustable with a pan-tilt and zoom head, allowing a consultant to study monitors. The remote consultant can grab scan images, send them down to the device by the bedside, and annotate them in real-time for the medical team with the patient. Boom cameras with a 36x zoom can look down on a patient in close detail. Consultants can also listen to a stethoscope to hear a heartbeat in real time.
Patient and clinician experience
Dr Jackson has been pleased by the patients’ reactions to the technology. He comments:
‘Patients are not fazed at all by the fact I’m on the screen. They are very positive about it when they give feedback, and the junior team loves it. Using a telemedicine device felt surprisingly natural, despite my initial concerns. I can also review patients who are admitted to my ward between my formal ward rounds, which means they may be discharged earlier.’
The telemedicine device relies on someone to take the device to the patient. The team can view a small image on the screen to see the consultant’s perspective. This means that if there’s a part of the patient’s body, the consultant needs to see if the team can assist. Dr Jackson gives an example of this:
‘As a diabetic foot doctor, I would normally have to get on my knees and look underneath the patient’s foot. With the telemedicine device, the team can lift the foot up for me, and they can see where to place the foot so I can view it myself without too much effort on my part!’
Increased access to specialists from other sites
Specialists at Leicester try to go to other departments to save a transfer of a patient from one site to another. However, this isn’t always practical–until now. Dr Jackson cites a recent example:
‘Patients had to wait for hours to be transferred from our emergency department to the hospital with cardiologists. I freed up some of my time to wheel this cardiologist into the emergency department on the telemedicine device. As a result, patients were discharged from ED, instead of having to wait for a bed at the other hospital, and the follow-up was organised in a timely fashion by this consultant on the screen.’
The news is spreading at University Hospital Leicester, with Dr. Jackson receiving inquiries from other specialties.
The consultant neurologist believes that telemedicine devices with a specialist on the screen can effectively diagnose patients, as the examination adds little to what the history provides. And if the examination is required, one of the other clinicians in the room can do it with the supervision of the specialist; they can make a plan with the patient, and so that there’s confidence all round.’