Next week, we will release our benchmark report incorporating nine years of data from June 2015 to June 2024.
Published around this time each year, our benchmark report is now the go-to for NHS professionals who are considering launching or refining Advice & Guidance (A&G) services.
This year’s trends include:
Now covering over 42 million patients across more than half of the NHS in England, Scotland and Wales, Consultant Connect works as a single point of access for clinicians to speak with NHS specialists for pre-referral Advice & Guidance (A&G).
Our services are available to over 10,000 consultants and 5,000 GP practices, and our data provides us with unique insight into the effectiveness of A&G in the NHS:
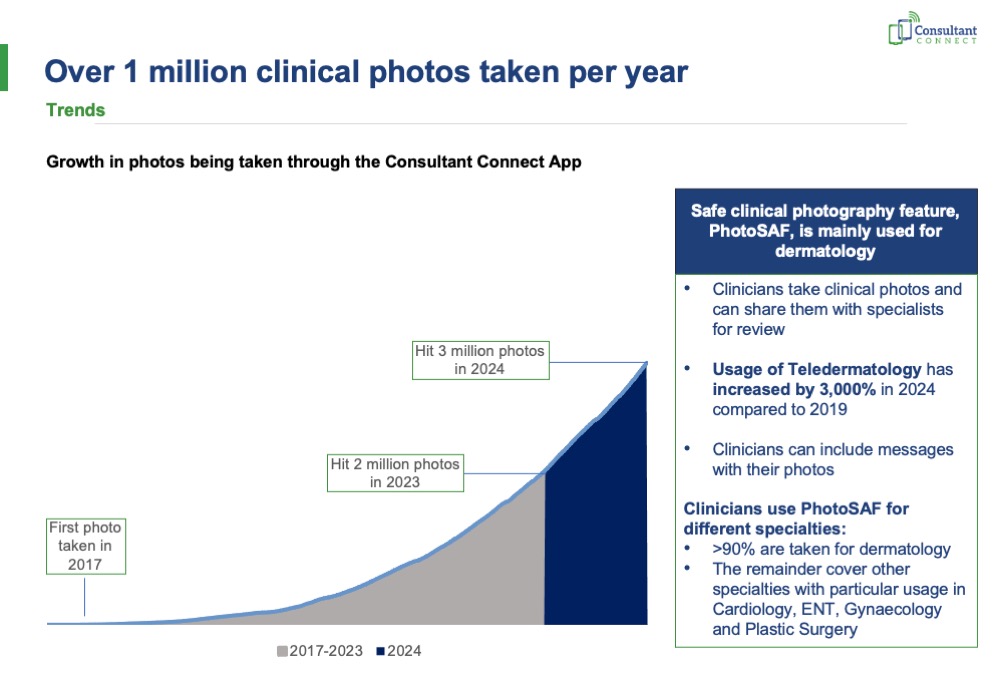
- 3 million clinical photos have been taken
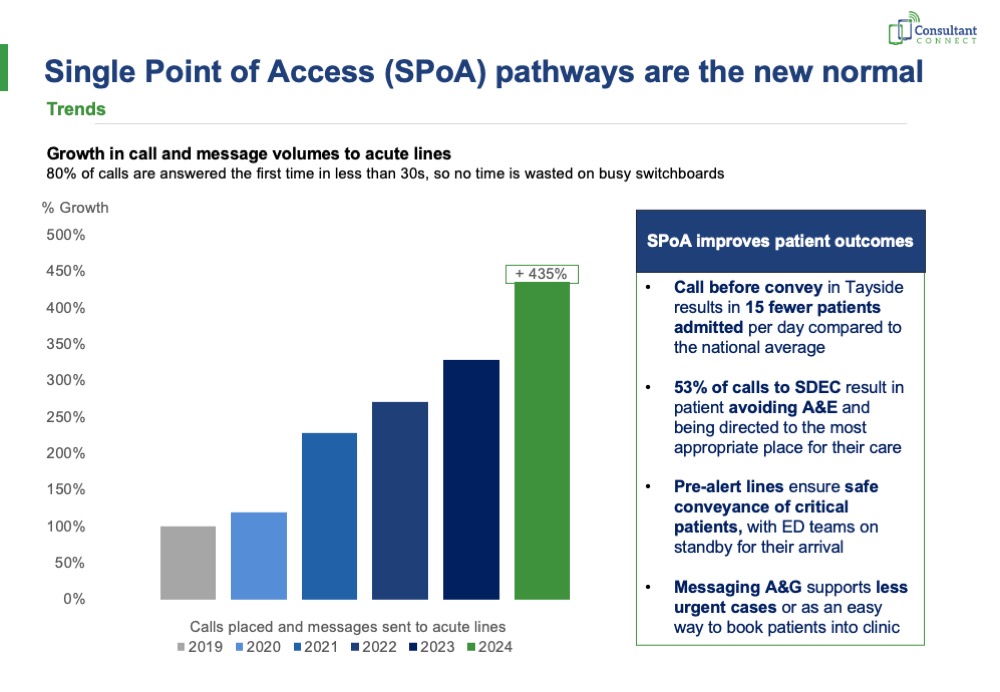
- 2 million calls have been placed
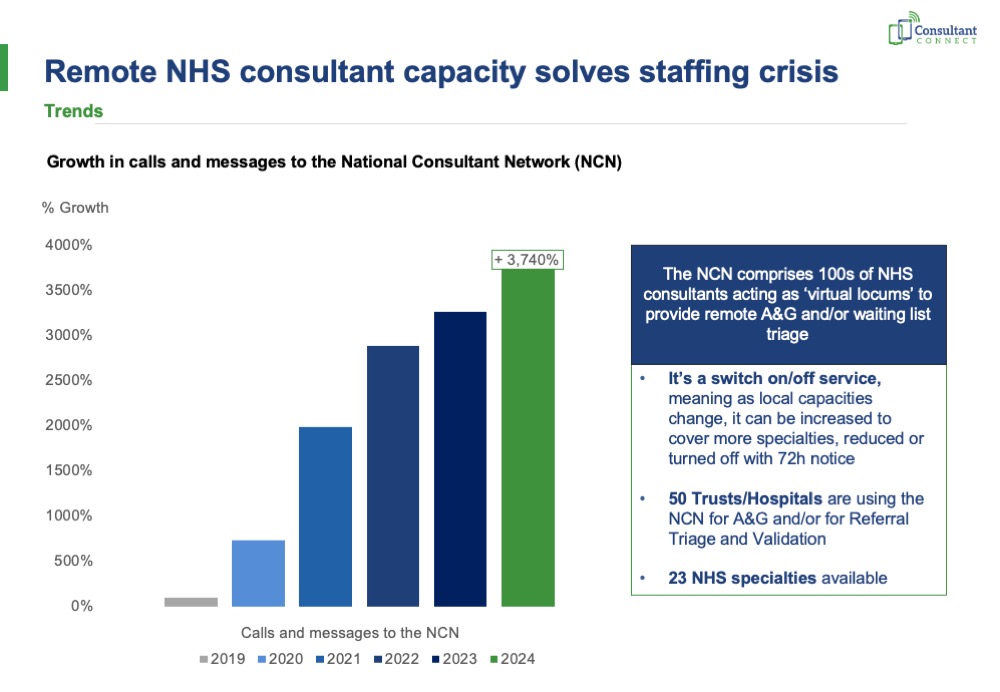
- 350,000 messages have been sent
Want to be the first to receive the aggregated Consultant Connect data from June 2015 to June 2024? Fill in the short form below: